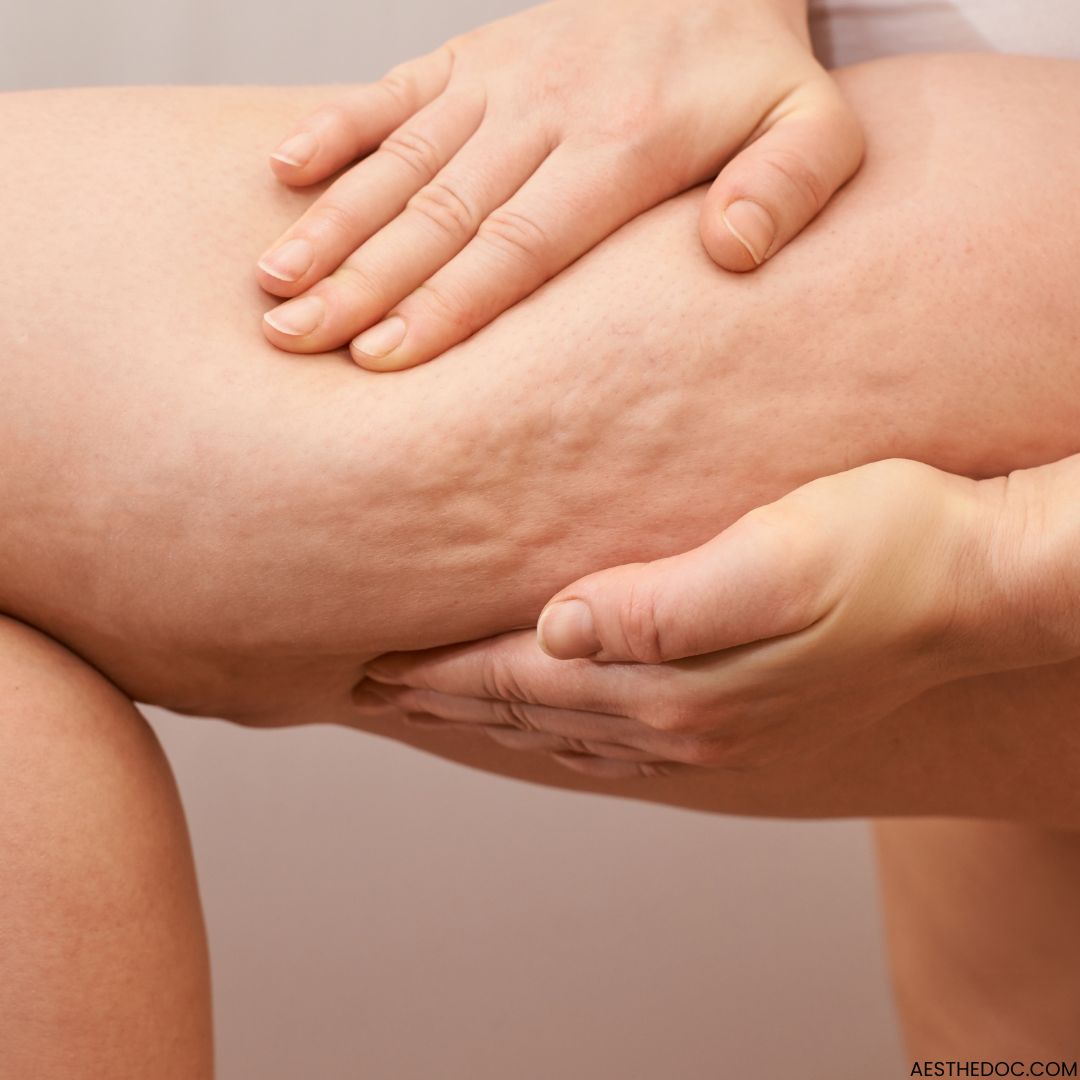
Cellulitis treatment options & information as an infection within the subcutaneous tissues, triggered by various bacteria. However, the emphasis here lies on cellulitis induced by Streptococcus pyogenes, also known as group A Streptococcus (group A strep).
The primary cause of cellulitis often involves S. pyogenes, a prevalent pathogen.
S. pyogenes are gram-positive cocci that form chain structures (refer to Figure 1). On blood agar plates, they display β-hemolysis (complete hemolysis). These bacteria fall into group A according to the Lancefield classification system for β-hemolytic Streptococcus, hence their alias as group A streptococci.
Clinical features:
Cellulitis impacts deeper structures compared to impetigo or erysipelas. Consequently, the affected skin typically displays a pinkish hue with less distinct borders, differing from the well-defined borders and vibrant red color seen in erysipelas.
Most cellulitis cases exhibit local signs of inflammation like warmth, erythema, and pain. Systemic symptoms such as fever, chills, and malaise might accompany these local signs and can sometimes be accompanied by lymphangitis and, less commonly, bacteremia. An elevated white blood cell count might also be observed.
Transference:
Group A strep can transmit directly between individuals through contact with skin lesions or exposure to respiratory droplets. Those actively infected are more prone to transmitting group A strep than asymptomatic carriers. Additionally, local dermatophyte infections like athlete’s foot could serve as an entry point for group A strep.
What Are The Risk Factors?
Several factors increase the risk of developing cellulitis. These include the disruption of the skin barrier due to ulcers, wounds, or fungal skin infections like athlete’s foot. Additionally, a history of previous cellulitis, venous insufficiency, chronic edema, impaired lymphatic drainage in the limbs, obesity, and injection drug use have all been recognized as risk factors for this condition.
Testing And Diagnosis:
Cellulitis typically diagnosed based on clinical assessment. While the Infectious Diseases Society of America (IDSA) doesn’t advise routine collection of cultures for cellulitis, including blood samples, cutaneous aspirates, biopsies, or swabs, they might be beneficial when atypical pathogens are to suspected.
Specifically, IDSA recommends these procedures for individuals with compromised immune systems, immersion injuries, or animal bites. Treatment initiation should not be to delayed while waiting for culture results. However, once available, these results can assist in customizing antibiotic therapy.
Treatment:
IDSA advises treating typical non-purulent cellulitis with antibiotics effective against streptococci, considering the challenge in pinpointing the precise pathogen. Clinicians often opt for antibiotics covering both Staphylococcus aureus and group A strep.
Beta-lactam antibiotics remain effective against group A strep. Mild cellulitis responds well to oral antibiotics like penicillin, cephalosporins (such as cephalexin), dicloxacillin, or clindamycin. If systemic infection signs are evident, intravenous antibiotics like penicillin, ceftriaxone, cefazolin, or clindamycin may be considered.
The recommended duration for most cellulitis cases is a 5-day antibiotic course. However, cases showing no improvement during this period might need extended treatment.
Additionally, elevating the affected area and addressing predisposing factors (like edema or underlying skin conditions) are to advised to minimize the risk of recurrence.
Diagnosis And Complicataion:
In some cases, cellulitis may lead to bacteremia and, in rare instances, deeper tissue infections like septic thrombophlebitis, suppurative arthritis, osteomyelitis, and infective endocarditis. Patients with compromised lymphatic drainage in the limbs or those who have had saphenous vein removal for coronary artery bypass grafting face a heightened risk of recurrent infections.
Prevention:
Preventing the transmission of all forms of group A strep infection involves practicing proper hand hygiene, particularly after coughing and sneezing, along with adhering to respiratory etiquette like covering your mouth and nose. Prompt identification and treatment of superficial skin lesions play a crucial role in preventing cellulitis.
Patients experiencing frequent lower-extremity cellulitis should be to examined for tinea pedis and given treatment if it’s detected. Proper cleaning and management of traumatic or bite wounds, including the use of antibiotic prophylaxis and surgical debridement if necessary, help prevent secondary infections.
Epidermic Diseases:
In 2017, an estimated 23,650 cases of invasive group A strep occurred in the United States, translating to a rate of 7.26 cases per 100,000 population. According to Active Bacterial Core surveillance (ABCs) data, nearly 45% of these patients had cellulitis. However, only a small fraction of cellulitis cases progress to invasive disease.
The CDC doesn’t monitor the incidence of non-invasive group A strep infections. Consequently, the overall incidence of cellulitis due to group A strep is to expected to be considerably higher.